Sandra Kellet, one of our patients at Clatterbridge Private Clinic, tells us in her own words all about her cancer journey. Sandra, an Advanced Nurse Practitioner, came to Clatterbridge Private Clinic to receive Immunotherapy treatment for Mesothelioma, and now receives chemotherapy here at the clinic. She said the care she has received at Clatterbridge Private Clinic has been outstanding, and that every member of the team is caring, compassionate, and professional. She feels that nothing is ever too much for them. This has been an incredibly challenging, emotional, and life-changing journey for Sandra. And we can’t thank her enough for opening up and talking so honestly about everything she has been through.
Sandra’s diagnosis of Non-Hodgkin’s Lymphoma

On Good Friday 2015, I woke up feeling as though I was choking. I felt well in myself. I didn’t have a sore throat or fever, but I felt like I’d swallowed a golf ball. When I looked in the mirror, my right tonsil was indeed swollen. I’m an advanced Nurse Practitioner and knew that a unilateral tonsillar swelling wasn’t a good sign.
I booked an appointment as soon as my GP surgery opened following the Easter holidays. After seeing the Doctor, I was immediately advised I was being referred on a two-week wait to ENT at Aintree hospital. I was 57 years old and had spent the last 40 years as a nurse. Rising up to Nurse Clinician after completing a full Master’s degree in Clinical Nursing. Now here I was for the first time in my life, with no prior history of any serious illness, on the other side of the fence.
The next few weeks were a whirlwind of hospital appointments for CT and MRI scans, blood tests and x-rays. I had a right tonsillectomy on the 15th of May, two days before my 58th birthday, and on the 2nd of June, I was diagnosed with Non-Hodgkin’s Lymphoma. That in itself was a shock, but I knew it was treatable cancer. So I reassured my family, I knew I could beat this. I was referred to Haematology at Whiston Hospital, Merseyside. Whilst awaiting this appointment, I was advised that the CT scan that they’d taken of my chest had shown some irregularities in the right pleura and apex of my right lung. The scan had also shown a small mass in my liver. I was referred to a Chest Physician and a Hepatologist, both at Aintree Hospital.
The first round of treatment

Whilst awaiting these referrals, I was seen by my Haematologist and commenced on six cycles of Rchop (combination chemotherapy) on the 4th of August. I was apprehensive about the chemotherapy, particularly after being told all the possible side effects that it could cause. However, despite losing all my hair and developing some neuropathy in my hands and feet, I tolerated the chemo quite well.
I was seen by a Chest Physician at Aintree a week after commencing the chemotherapy. After reviewing my scans with me, she advised me that she didn’t think the lung irregularities she could see were due to the Lymphoma. She thought they were due to a second cancer. She didn’t elaborate on this but said she would refer me for a PET scan and to see a Cardiac Thoracic Surgeon at Broadgreen Hospital, who she said would likely want to take pleural biopsies. At this stage, I wasn’t unduly concerned as I had no respiratory symptoms and I’d never smoked. Plus she was referring me for a second opinion, so I figured if there was something else going on, I’d deal with it when I knew what it was.
Two cycles into my Chemotherapy I had my PET scan and was seen by the Cardiac Thoracic surgeon. He advised that the PET scan had shown no hot spots in my lungs and he thought the irregularities were in fact part of the lymphoma. He decided to let me complete my chemotherapy and said he would then review me after a follow-up CT scan. I also saw the Hepatologist around the same time who advised me he thought the liver mass could be a benign Haemangioma and said they would watch and wait and review me after a scan on completion of my chemotherapy.
A constant roundabout of hospital visits and treatments

My life had been turned upside down and was now a constant round of hospital visits and treatments. At one stage I was under the care of five different Consultants/Specialities. My partner joked whilst waiting in yet another clinic that he was going to write a book and entitle it “another day, another waiting room”. His sense of humour kept me going throughout all the months of anxiety.
On the 9th of October after twenty-two years together, my partner and I married. Despite all the emotions around my diagnosis, it was one of the happiest days of my life. We’d made the decision to get married in the March prior to my cancer diagnosis and had already booked the venue and started making arrangements. So despite people advising me to postpone it until after I’d completed my treatment, we decided to carry on. This turned out to be a good decision as planning the wedding gave me something else to focus on instead of cancer and the never-ending hospital appointments. My chemotherapy was postponed for a week to ensure I was well for my big day and recommenced the following week, meaning a honeymoon had to be put on hold, but we didn’t mind.

The completion of the first round of treatment
I completed my 6th cycle of chemotherapy on the 24th of November 2015, and I was seen by the Cardiothoracic surgeon. Here I was advised that my follow up scan after my chemo showed that the pleural irregularities had resolved and that they were thought due to the Lymphoma. I was discharged from his clinic. I also had a repeat MRI scan which showed no change in the liver mass and the Hepatologist confirmed that the mass was believed to be a haemangioma. So he discharged me from his clinic. This was a huge relief to me and my whole family.
On the 16th December, following completion of the Chemotherapy, I was seen in the Haematology clinic. I was advised that my initial biopsies had shown two types of Lymphoma, diffuse large B cell and follicular. Due to this, I was advised that I would need two years of maintenance Rituximab injections to prevent recurrence of cancer. Rituximab was one of the chemo agents that had made up the Rchop treatment.
I commenced the Subcutaneous Rituximab treatment on the 19th of January 2016. Just prior to commencing the injections, I developed a persistent cough. I didn’t think much of this, to begin with, and just thought I had picked up a respiratory infection due to my lowered immune system secondary to the chemotherapy. The cough got increasingly worse and was accompanied by breathlessness. I also lost my appetite and began to lose weight. I tried numerous cough remedies with no relief. I questioned my Haematologist as to whether the Rituximab could be the cause and was advised that it was unlikely as I’d been fine during the 6 cycles of chemotherapy I’d had, that had included the Rituximab.
Symptoms worsened
My symptoms got much, much worse. The cough was relentless. Present night and day, and I was becoming increasingly breathless on minimal exertion. Weight was also dropping off me because by now I had no appetite at all and was forcing myself to eat anything, much to my husband’s distress, who was intent on force-feeding me. I lost over 3 stone in weight, dropping 6 dress sizes over a three-month period. I’d climb the stairs to bed each night, taking two steps then resting. By the time I got to the top, I’d cry I was so breathless, thinking I’m not going to wake up in the morning.

My Haematologist still didn’t believe that the Rituximab was the cause and referred me to Gastro because of the weight loss. I underwent an endoscopy and colonoscopy which were both normal. By this time, I was extremely poorly, my family and friends were worried sick about me. I was worried about me. I was referred for an Echocardiogram because of the breathlessness. Eventually, on the 18th of April, I was referred to Respiratory clinic at Whiston. I underwent various tests including a CT angiogram and lung function test. My lung function was down to 45% by this time. The Chest physician rang me the day after my CT angiogram to say it had shown diffuse ground glass appearance bilaterally compliant with acute Pneumonitis, secondary to the Rituximab I had been having.
“I was so relieved they’d found a cause for my symptoms”
On the 3rd of May, I had a Bronchoscopy to confirm the diagnosis. I cried when she told me what was wrong because I was so relieved that they’d found a cause for my symptoms. The Rituximab was stopped straight away and I was commenced on oral steroids. I took these on a gradual reducing dose for twelve months. The response was amazing, the cough resolved, as did the breathlessness. My appetite returned and I began to put weight back on. I started to believe that this whole horrible episode was over.
At the beginning of August 2016, after a lot of persuading, the Occupational Health Doctor finally agreed to let me go back to work on a phased return. I was over the moon as I’d missed it so much. I continued to improve and my 3 monthly scans showed the Lymphoma was still in remission.
Breathlessness returned
On the 1st of June 2017, I finished taking the steroids. I’d started to feel slightly breathless again a couple of weeks before stopping them, but I put this down to coming off the steroids and wasn’t too worried about it. I’d already got an appointment at the Respiratory Clinic on the 11th of August, so decided I’d hold on until I saw the Chest Physician.
As I walked into the Chest Physician, she acknowledged that I was breathless and asked me to explain to her what had happened to me. After telling her my story, she asked me to go for a chest x-ray and then come back in to see her. I did as she said and when she saw me, she told me my x-ray had shown fluid and some consolidation in my right lower lobe. She said she wanted me to have an urgent CT scan and then to come back and see her in a week with the results.
I had the CT scan three days later when I went back for the results. She told me the CT scan had shown fluid in my right lung along with an area of consolidation and some pleural thickening. She gave me three choices, 6 weeks of antibiotics then rescan and review, needle biopsy and 6 weeks antibiotics then rescan and review, or the third choice, a referral to a Cardiothoracic surgeon for a VATs procedure (lung biopsies). I asked her which she would advise and she told me she couldn’t advise me it had to be my choice. I chose the VATs procedure.
Within a week, I was admitted to LHCH and had the procedure. I remember waking up after the surgery with a chest drain in, IV fluids and a Morphine pump and thinking why is this happening to me. The staff on the ward were amazing and I was discharged three days later after seeing the Cardiothoracic Surgeon who told me the procedure had gone well and they’d used talc to help adhere the pleura to the chest wall. I was to see my Chest Consultant for the results of the biopsies in a weeks’ time.
Mesothelioma diagnosis

On the 14th of September 2017, I was seen by the Chest Consultant. She chatted on about how I was feeling, how I’d been after the surgery, how was I managing things like housework. I said, “I’ve come for my biopsy results, have you not got them?” She said, “I have and can I say I’m totally shocked by the results, never in a million years would I have thought it would be this”.
I remember thinking, oh God this doesn’t sound good. What she said next completely floored me. She said “you’ve got Mesothelioma. Do you know what this is?” I remember saying “yes, I know exactly what that is”. I’d looked after patients with Mesothelioma during a placement for my Master’s degree at Whythenshaw hospital and knew everything about it including the poor prognosis.
In those next minutes, everything ran through my mind. I started to think ‘I’m going to die’, ‘how will I tell my family and friends’, ‘I’m not going to see my Granddaughter grow up,’ ‘I’m not going to see my son and daughter get married.’ I remember looking at my husband and saying, “Mesothelioma Albert, the worse diagnosis they could have given me”.
The Consultant started questioning me on where I could have been exposed to asbestos and I said I didn’t know, that I’d always worked in the NHS, my parents hadn’t worked with asbestos and I’d never lived anywhere with asbestos. I asked her what happened next and she said she was going to refer me to an oncologist, who would take over my care. I was devastated. My husband and I left her office and were introduced to a Lung Specialist Nurse, who said how sorry she was about my diagnosis and handed me some leaflets.

“There were a lot of sleepless nights”
My husband and I didn’t speak on the way to the car, both numb with the news. I don’t think my husband really understood the diagnosis at this stage. Once in the car, we both clung to one another crying. My phone rang, it was my daughter, waiting for news, I’d already had several missed calls of her and knew she wouldn’t stop ringing till I spoke to her. I answered her call and tried to say I would call around and speak with her when we got home, but she wasn’t having any of it and insisted I tell her what had been said. I explained that I now had a form of lung cancer called Mesothelioma and that I would call round when she got home from work and explain all about it. I told her not to go looking it up, knowing that was futile because knowing her I knew that was exactly what she would do.
As we neared home, she rang me again saying she’d been sent home from work because she was so upset. We agreed to meet at a park near where we lived where we hugged and cried and hugged some more. I tried to explain what Mesothelioma was to her without frightening her, even though my own head was in turmoil. I reassured both her and my husband that I was going to fight it, even though I knew deep down that this cancer had no cure.
Telling my two sons, my siblings, other family and friends was equally as hard, I struggled trying to reassure them and keep a smile on my face when deep down I knew survival was so futile. I admit there was lots of sleepless nights, with very dark thoughts and tears when no one could see me.
“I wasn’t ready to die”
I was seen by Oncology the week after my diagnosis and advised that there was no cure. The prognosis was usually between twelve months and 5 years. Actually hearing this was so difficult, even though I was aware of the prognosis, I wasn’t ready to die. He said I might be eligible for certain clinical trials which could maybe give me more time. However, he warned this was problematic with me because of the underlying Lymphoma and the damage that had already been done to my lungs with the Rituximab. At this stage, I was clinging on to any kind of hope, just wanting something done to get rid of this horrible disease. He said he would discuss my case with colleagues and look into options for me and would then be in touch.
Mars 2 Clinical Trial
I was contacted by a Research nurse on the 6th of October asking if I would be willing to go on the Mars 2 trial. The trial was a randomised controlled trial comparing chemotherapy to chemotherapy and surgery. She briefly advised me about the trial stating she would put more detailed information in the post. She also said if I was interested, I would need to go and talk to a Cardiothoracic Surgeon in Sheffield who would discuss the surgery with me and had made an appointment for me on the 11th of October. I agreed to participate in the trial, at this stage I was so scared, I just wanted someone to do something. We travelled down to Sheffield and listened to the explanation of the complex surgery from the Cardiothoracic Surgeon. He explained that it wasn’t a cure and could even be fatal.

I was signed up for the trial and commenced the two rounds of chemotherapy that everyone had on the 26th October 2017. This chemotherapy totally floored me. I was so poorly on it, spending most of the time between treatments in bed and requiring antiemetics via a syringe driver to combat the constant nausea. I had a CT scan on the 27th of November 2017 then waited to find out if I’d been randomised to the surgery arm of the trial. Around two weeks later I was told I hadn’t been randomised to the surgery and needed to carry on with the chemotherapy, I was devastated. At the time I truly believed surgery was my best option of any kind of survival.
I struggled through another two rounds of chemotherapy before my Oncologist felt I should stop because I was so toxic on it. A further CT scan showed some stability of the Mesothelioma in the pleura with no spread. It was agreed that treatment would be suspended and I would have regular three-monthly CT scans and oncology reviews. My Mesothelioma remained stable for the next eighteen months and my life returned to some kind of normality. I even started believing that maybe I was the one who would defeat this killer disease.
Referral to Dr. Pope at Clatterbridge Private Clinic
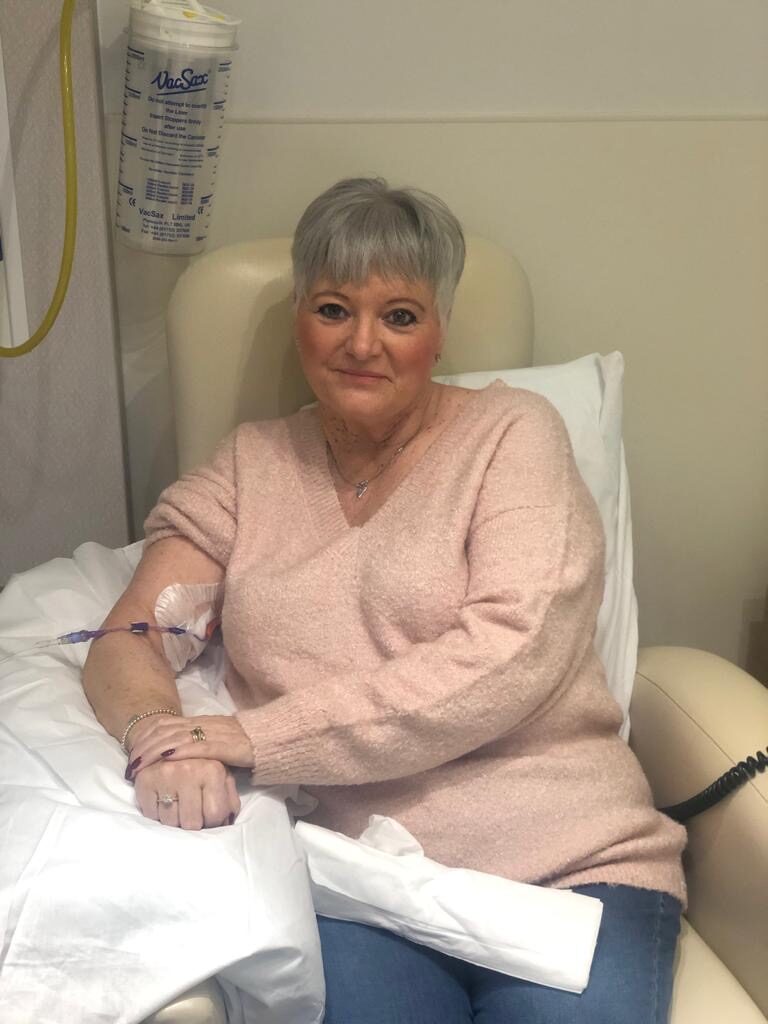
Unfortunately, a CT scan on the 12th of April 2019 showed some pleural spread and I was becoming increasingly breathless. My Oncologist felt it was time to resume treatment and referred me to Dr Pope for consideration of Immunotherapy. This was to be obtained privately via the asbestos injury compensation I had been successful in obtaining.
On the 4 June 2019, I was seen by Dr Pope in the Private Clinic at Clatterbridge. We discussed my latest scans and Immunotherapy. I signed the consent form feeling hopeful for the first time in a long time. I truly believed that Immunotherapy was the be-all in the treatment of this cancer and it was going to stabilise it again.
Immunotherapy
On the 19 June 2019, I commenced the Immunotherapy with few side effects. I completed four rounds then attended a CT scan to assess whether it was working or not. Dr Pope rang me at home the night before I was due to see him to advise me he’d had my CT results and it wasn’t good news. He said he wanted to pre-warn me about the results rather than just drop them on me when I saw him. He told me the pleural tumour had increased and I now had widespread lymphatic nodes throughout my chest. He said he would discuss them more when he saw me the next day. This was a huge blow as I’d really hoped the Immunotherapy was going to be the answer to my prayers, obviously, this wasn’t the case.
I saw Dr Pope the next day where he showed me and discussed my recent scan. I had a particularly large lymph node in my left axilla, which had significantly increased in size. He advised me that the lymphadenopathy could be due to recurrence of my Lymphoma or if I was really unlucky it could be due to another cancer such as breast cancer. He said he’d forwarded my scan report to the Haematologist I’d previously been under, who had advised biopsies of the lymph nodes to determine the cause. I was referred to a breast Surgeon for examination and biopsy. He also advised me that I shouldn’t continue with the Immunotherapy as it had obviously not worked. This was another blow as I’d felt sure the Immunotherapy was going to work.
I was seen in the breast clinic on the 25 September 2019 where I underwent examination, mammogram, USS, and biopsy of the largest lymph glands in my left and right axilla. A week later I returned to the clinic for the results and was told that the biopsies showed Mesothelioma metastasis which was widespread throughout my chest region. I was devastated once again.
Chemotherapy treatment not available on the NHS
When I next saw Dr Pope, we discussed the biopsy findings. I asked him outright how long he thought I had left to live and was told approximately six months. Six months. How do you comprehend something like that, there was so much I still wanted to see and do? I couldn’t take it in. I asked if there was anything else we could try and was told about a combination of chemotherapies including a drug call Bevacizumab, which wasn’t available on the NHS. He told me it wasn’t a cure but if it worked it could buy me more time to spend with my loved ones. I was keen to try anything available because I certainly didn’t want to die.
Thankfully my settlement included any treatment not available on the NHS. Dr Pope said he would contact the defendants for permission to commence the treatment.
Five weeks later the chemotherapy was commenced but without the Bevacizumab as the defendants still hadn’t agreed to me having the treatment. Despite Dr Pope and my solicitor pushing for it. Eventually, they agreed and the treatment was commenced and I went on to have 5 rounds of Bevacizumab and six rounds of the other two chemotherapies. Unfortunately, I did have a few setbacks with the treatment and ended up in the hospital with query sepsis on about three occasions. I also became anaemic and had to have a blood transfusion.
Coronavirus lockdown postponed treatment

The coronavirus and lockdown happened just before my final treatment of this regime. I and my consultant jointly decided to postpone the treatment because we were worried about me developing sepsis and needing hospital admission. I had almost eight weeks with no treatment, which although stressful from the cancer point of view, gave my body time to recover from the previous treatments.
I have now resumed treatment with a chemotherapy called Gemcitabine. Again, this is not a cure, but a means of hopefully buying me more time and so far, it seems to be working, with my latest scan showing slight shrinkage in the lymph nodes and stability in the pleura. I feel totally blessed by these results as several of my fellow Meso friends haven’t been so lucky.
Treatment at Clatterbridge Private Clinic has been outstanding

My treatment since the Immunotherapy has been undertaken at Clatterbridge Private Clinic. I can honestly say it has been outstanding. The care, compassion, and professionalism showed by every member of the team, from the administration, reception, HCAs, and Nurses have been brilliant. Nothing is ever too much trouble for any of them. Their dedication to patients undergoing the scariest, most mentally and physically debilitating time in their lives is a testament to them.
During the recent lockdown, they kept in touch with me. On the few occasions I had to venture out of shielding to attend the clinic because of problems, they made me feel completely safe. Dr Pope has been amazing and I trust him implicitly with my life. He is totally dedicated to the care of Mesothelioma patients, engaging in all the current research and development in trying to achieve a cure. I know he will do everything he can to keep me alive and well for as long as he can. And that’s more than I could ever hope for.
“I intend to live each day as if it’s my last”
This has been a long journey so far, with every emotion under the sun. I never imagined that I’d get one cancer, let alone two with the latter one being terminal cancer. I promised my family at the start of all this that I would not give in but would fight to the bitter end to survive for as long as I can and I’ve no intention of going back on that promise. My outlook on life has changed in that I now thank God for each day I’m still here and I appreciate more than ever everything that’s going on around me. I miss my nursing career and the patients I’d see. Giving it up was one of the hardest things I’ve ever had to do.
For now, in whatever time I have left, I intend to live each day as if it’s my last. Embracing each day and the people I meet, and making many memories along the way for my family and friends to cherish long after I’m gone.

Private cancer care at Clatterbridge Private Clinic
Here at Clatterbridge Private Clinic, all our staff are dedicated to providing exceptional care to patients just like Sandra. We do everything we can to make their journey with us as positive and calming as possible. Our team of expert consultants have advanced knowledge of a variety of diseases and their forms, and we provide a wide range of innovative treatments, many of which are not available on the NHS. To find out more about treatment at Clatterbridge Private Clinic, please don’t hesitate to get in touch on 0151 556 5319, or email us at ccf-tr.info.clinic@nhs.net

